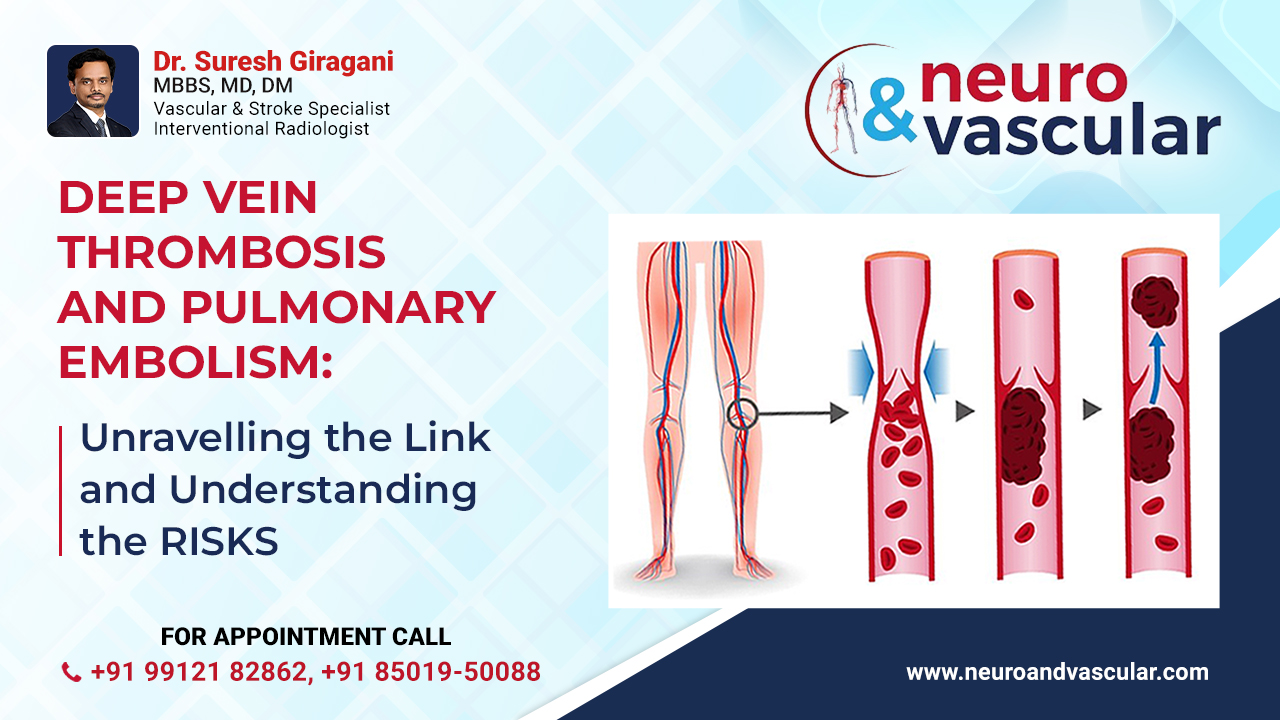
Deep Vein Thrombosis and Pulmonary Embolism: Unravelling the Link and Understanding the Risks
Deep Vein Thrombosis (DVT) and Pulmonary Embolism (PE) are two interconnected and potentially life-threatening conditions that involve blood clot formation within the circulatory system. In this blog, we’ll delve into the intricacies of DVT and PE, exploring their link, symptoms, risk factors, and preventive measures.
Deep Vein Thrombosis occurs when a blood clot forms in a deep vein, usually in the legs. The clot can impede or completely block blood flow, leading to various complications. DVT is often associated with prolonged immobility, surgery, or medical conditions that affect blood clotting.
Symptoms of DVT:
- Swelling in the affected leg, often accompanied by pain or tenderness.
- Warmth and redness in the affected area.
- Swelling and discoloration of the skin.
Understanding Pulmonary Embolism (PE):
Pulmonary Embolism is a serious condition that occurs when a blood clot, usually from the legs (DVT), travels to the lungs and blocks one of the pulmonary arteries. This sudden obstruction can be life-threatening, compromising the ability of the lungs to oxygenate the blood.
Symptoms of PE:
- Sudden shortness of breath.
- Chest pain that may become worse when breathing deeply, coughing, or even swallowing.
- Rapid heart rate.
- Cough that may produce bloody or discolored sputum.
The Link between DVT and PE:
DVT and PE are interconnected in what is known as venous thromboembolism (VTE). When a blood clot forms in the deep veins (DVT), it can break loose and travel through the bloodstream to the lungs, causing a pulmonary embolism. The risk of PE is significantly increased in individuals with untreated or undiagnosed DVT.
Risk Factors for DVT and PE:
1. Prolonged Immobility:
• Long flights or car rides.
• Extended bed rest.
• Immobility after surgery.
2. Surgery and Hospitalization:
• Certain surgical procedures, especially those involving the lower extremities.
• Extended hospital stays.
3. Medical Conditions:
• Cancer.
• Inherited blood clotting disorders.
• Inflammatory conditions.
4. Pregnancy and Postpartum Period:
• Pregnancy increases the risk of blood clot formation.
• The postpartum period is associated with an elevated risk.
5. Age and Gender:
• Older age.
• Women, particularly during pregnancy, postpartum, and while taking hormonal contraceptives.
Preventive Measures:
1. Stay Active:
• Regular exercise promotes healthy blood circulation.
2. Maintain a Healthy Weight:
• Obesity is a risk factor for DVT and PE.
3. Hydration:
• Staying hydrated helps prevent blood from thickening.
4. Avoid Prolonged Immobility:
• Take breaks during long flights or car rides.
• Perform leg exercises when sitting for extended periods.
5. Medical Intervention:
• Anticoagulant medications may be prescribed in certain situations.
• Compression stockings can help prevent DVT.
Deep Vein Thrombosis (DVT) is a medical condition that occurs when a blood clot forms in a deep vein, typically in the legs. If left untreated, DVT can lead to serious complications, such as pulmonary embolism. Post thrombotic syndrome which is severe disability effecting people with chronic unresolved DVT is a quality of life limiting complication of DVT, in which the effected person develops severe pain, swelling of the effected leg on short distance walking. There will be associated skin discoloration, itching, dermatitis, ulcer formation.
Understanding Deep Vein Thrombosis:
Deep Vein Thrombosis occurs when a blood clot, or thrombus, forms in a deep vein. The clot may impede or block blood flow, leading to pain, swelling, and other symptoms. DVT is associated with factors such as prolonged immobility, surgery, trauma, and certain medical conditions, making it imperative to identify and manage the condition promptly.
The Risk of Pulmonary Embolism
One of the most severe complications of DVT is pulmonary embolism (PE), which occurs when a blood clot dislodges from the veins and travels to the lungs. PE can be life-threatening, causing difficulty breathing, chest pain, and, in severe cases, cardiac arrest. Timely intervention is essential to prevent the progression from DVT to PE.
Thrombolysis:
Thrombolysis, also known as fibrinolysis or clot-busting therapy, is a medical procedure designed to dissolve or break down blood clots. This intervention is particularly relevant in the context of pulmonary embolism when the goal is to prevent further clot growth, reduce symptoms, and minimize the risk of complications.
Catheter directed thrombolysis and mechanical thrombectomy
DVT Catheter directed thrombolysis is typically performed in a hospital setting by a specialized healthcare team. The procedure involves the administration of thrombolytic medications, which are powerful enzymes capable of dissolving blood clots. These medications may be delivered directly into the clot through a catheter. Catheter-directed thrombolysis is a targeted approach where a catheter is guided to the site of the clot, allowing for the precise delivery of the thrombolytic medication. This method minimizes the risk of systemic bleeding and enhances the efficacy of the treatment.
In mechanical thrombectomy a large bore aspiration catheter is navigated into the clot in the deep veins or pulmonary arteries and the clot is sucked out using vaccum effect. It avoids the use of any thrombolytic drug and its associated side effects are therefore eliminated.
Benefits and Risks
The benefits of DVT thrombolysis are evident in its ability to rapidly restore blood flow, alleviate symptoms, and reduce the risk of complications. However, like any medical intervention, thrombolysis or mechanical thrombectomy comes with potential risks, including bleeding. The healthcare team carefully evaluates each patient’s case to weigh the potential benefits against the risks and determine the most appropriate course of action.
Conclusion:
DVT catheter directed thrombolysis and mechanical thrombectomy play a crucial role in the management of Deep Vein Thrombosis, preventing the progression of the condition and reducing the risk of acute life-threatening complications such as pulmonary embolism and mitigating the risk of chronic complications of DVT such as post thrombotic syndrome. Timely diagnosis, expert medical intervention, and a thorough understanding of the benefits and risks associated with these interventions are paramount in ensuring optimal outcomes for individuals facing DVT.
About the Author:

Name: DR . SURESH GIRAGANI
INTERVENTIONAL RADIOLOGIST
DR. SURESH GIRAGANI CONSULTANT INTERVENTIONAL RADIOLOGIST at Apollo hospitals Jubilee Hills has more than sixteen years of clinical experience in vascular interventions with a special interest in neurovascular and peripheral vascular disease interventional procedures.